If you’re in your third trimester, there’s a moment that’s hard to forget — the first squeeze across your belly that makes you stop mid-sentence and ask, “Wait… was that a contraction?” For decades, the answer relied on a stopwatch, a notebook, and a lot of guessing. Today, a contraction monitor can do that work for you, quietly tracking the rhythm of your body and giving you (and your doctor) real, useful data.
This guide breaks down everything you actually need to know: what a contraction monitor is, how the different types work, when they’re worth using, what the research says about accuracy, and how to choose one that fits your pregnancy. No fluff, no fear-mongering — just the practical, well-sourced answers parents-to-be keep searching for.
What Is a Contraction Monitor?
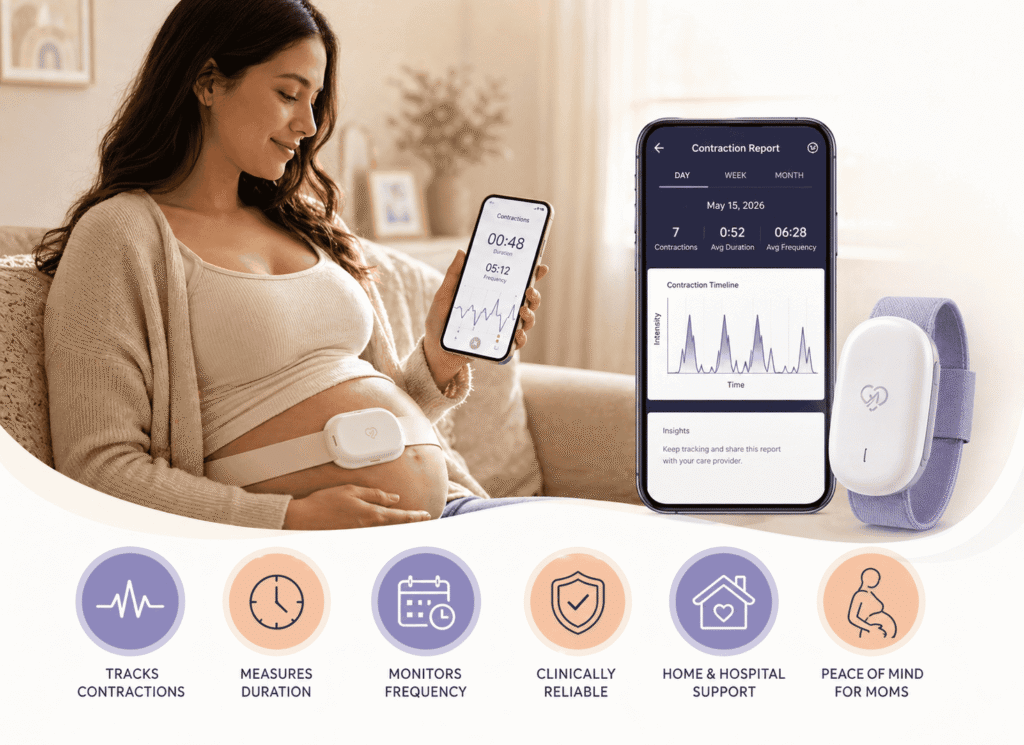
A contraction monitor is a device — medical or consumer — that detects, measures, and records the tightening of your uterine muscles during pregnancy or labor. Some monitors also track the fetal heart rate at the same time, which is why you’ll often hear them grouped under the broader category of fetal monitoring.
In a hospital, the standard tool is a tocodynamometer (often shortened to “toco”), a pressure-sensitive disc strapped to the abdomen. It’s typically paired with a Doppler sensor to capture baby’s heartbeat — together that combination is called cardiotocography (CTG) or, more commonly in the U.S., electronic fetal monitoring (EFM).
At home, the landscape looks very different. Modern wearable monitors and smartphone-paired patches use electromyography (EMG) — they read the tiny electrical signals your uterine muscle produces when it contracts. That’s a fundamentally different (and often more comfortable) approach than the strap-and-pressure method used in the hospital.
Quick definition for voice search: A contraction monitor is a device that detects when your uterus tightens, measures how long each contraction lasts, and tracks how often they happen — helping you and your healthcare team understand whether you’re in true labor.
How a Contraction Monitor Actually Works
Three core technologies power today’s contraction monitors:
1. Tocodynamometry (Pressure-Based)
Used in nearly every hospital labor and delivery unit. A belt with a pressure sensor sits on the upper part of your abdomen, where the fundus of the uterus is strongest. When the muscle contracts, the abdominal wall pushes outward, and the sensor records that change. It tells you frequency and duration, but not the true intensity of the contraction (only an internal pressure catheter can do that).
2. Electromyography (EMG-Based)
The technology behind most wearable home monitors. Skin-contact electrodes pick up the natural electrical activity that travels through your uterine muscle whenever it contracts. EMG is sensitive enough to register subtle Braxton Hicks as well as full active-labor contractions, often with no belt pressure required.
3. App-Only “Contraction Timers”
These aren’t really monitors — they’re manual timers. You tap a button when a contraction starts and again when it ends. The app does the math (frequency, duration, intervals). They’re free, they’re useful, and they’re the most common entry point for first-time parents.
Hospital vs. Home: Which Type Do You Need?
| Feature | Hospital Monitor (CTG / Toco) | Wearable Home Monitor | Phone Timer App |
|---|---|---|---|
| Detects contractions automatically | Yes | Yes | No (manual) |
| Tracks fetal heart rate | Yes | Some models | No |
| Comfort over long periods | Moderate | High | High |
| Clinical accuracy | Highest | Moderate to high | N/A |
| Cost | Covered by hospital | $200–$400+ | Free–$10 |
| Best for | Active labor, high-risk pregnancy | Late pregnancy, peace of mind | Early labor at home |
For most low-risk pregnancies, a free contraction timer app is genuinely all you need until you’re ready to head to the hospital. A wearable home monitor becomes valuable when there’s a clinical reason — a history of preterm labor, gestational complications, or simply high parental anxiety that interferes with sleep and daily function.
Braxton Hicks vs. Real Contractions: What a Monitor Will (and Won’t) Tell You
This is one of the most-searched questions in late pregnancy, and a monitor only solves half of it.
Braxton Hicks contractions — sometimes called “practice contractions” — are usually:
- Irregular and unpredictable
- Painless or only mildly uncomfortable
- Eased by changing position, hydrating, or resting
- Felt mostly in the front of the abdomen
True labor contractions are usually:
- Regular and progressively closer together
- Increasing in intensity over time
- Unaffected by movement, hydration, or rest
- Felt as a wave starting in the back and wrapping around to the front
A contraction monitor reliably records the timing pattern — and that pattern is the single biggest clue. If contractions are coming every 10–15 minutes and stay that way for hours, that’s likely Braxton Hicks. If they’re coming every 5 minutes, lasting 60 seconds, for an hour straight — that’s the famous 5-1-1 rule and it’s time to call your provider.
The 5-1-1 Rule (and Why a Monitor Makes It Easier)
The 5-1-1 rule is the most widely taught threshold for heading to the hospital with a low-risk, full-term pregnancy:
- 5 minutes apart
- 1 minute long, each contraction
- For at least 1 hour straight
Trying to track this manually while also breathing through contractions is exactly why monitors and timer apps exist. A good contraction monitor will graph this pattern in real time, so you stop second-guessing the math and start trusting what the screen shows you.
Important: Always follow your own provider’s guidance. Some practitioners use 4-1-1 instead, and anyone with a high-risk pregnancy, twin pregnancy, prior C-section, or VBAC plan may have a personalized threshold.
Are Home Contraction Monitors Accurate?
Short answer: for tracking patterns, yes. For predicting exactly when labor will start, no — and no monitor on the market can do that.
Peer-reviewed studies on consumer EMG-based monitors (like Bloomlife and similar wearables) have shown strong agreement with hospital tocodynamometers for detection of contraction events in third-trimester pregnancies. They’re considered reliable enough for awareness and pattern tracking — not for diagnosing labor, ruling out complications, or replacing professional care.
The bigger limitation is the same one hospital toco devices have: external monitors can tell you a contraction is happening and how long it lasts, but they cannot reliably tell you how strong it is. That’s clinical-grade information that requires an internal monitor placed by a provider after your water has broken.
When a Contraction Monitor Is Genuinely Worth It
There’s no need to over-equip a low-risk pregnancy. But here are the situations where a wearable monitor adds real, defensible value:
- History of preterm labor — Your provider may want extra data points between appointments.
- High-anxiety pregnancy after loss — A monitor can replace constant fetal kick-counting with calmer, structured awareness.
- Long-distance from your hospital — Earlier, more confident decisions about when to leave home matter more.
- Twin or multiple pregnancy — Higher baseline risk of preterm contractions.
- First-time parents who want a learning tool — Watching your own patterns helps you recognize real labor when it arrives.
What to Look for When Choosing a Contraction Monitor
Cut through the marketing with this checklist.
- FDA registration or CE mark. This is a non-negotiable for anything claiming medical use.
- Automatic detection, not manual tapping. If you have to push a button, it’s a timer, not a monitor.
- Continuous wear comfort. Look for soft, skin-friendly patches or belts you can keep on while sleeping.
- Long battery life. Late-pregnancy nights are not the time to fight a charging cable.
- Clear data export. Your OB or midwife should be able to actually use the report.
- No alerts disguised as diagnoses. A trustworthy device says “contraction detected” — not “you are in labor.” That call belongs to your provider.
Best Contraction Monitor & Tracker Categories in 2026
Rather than a brand ranking — which changes month to month — here’s how the market currently divides up. Match your situation to the category, then research the latest models in that tier.
1. Free / Low-Cost Contraction Timer Apps
Best for: most first-time parents, early labor at home. What they do well: Frequency, duration, and interval tracking with one-tap simplicity. What to skip: Apps that push paid “predictions” or fear-based notifications.
2. Wearable EMG Monitors
Best for: third-trimester tracking, anxious parents, history of preterm labor. What they do well: Passive, comfortable, data-rich. What to verify: Regulatory clearance and study-backed accuracy claims.
3. Combined Fetal Heart Rate + Contraction Monitors
Best for: medically supervised home monitoring. What they do well: Provide a fuller clinical picture. What to know: Many require a prescription or provider partnership.
4. Hospital-Grade Rentals
Best for: short-term medical need (e.g., bed rest, post-procedure observation). What they do well: Clinical-tier reliability at home. What to know: Cost is significant; insurance may cover with a referral.
How to Use a Contraction Monitor at Home (Step-by-Step)
- Position it correctly. EMG patches sit on the lower abdomen; tocos sit higher. Always follow your specific device’s placement diagram.
- Track in a calm baseline state first. Sit or lie still for 10–15 minutes so the device learns your resting pattern.
- Note context, not just data. A simple log — “big walk at 6pm, contractions started at 6:45” — turns numbers into a story your provider can act on.
- Hydrate and reposition before reacting. True labor contractions ignore both. Braxton Hicks usually fade.
- Know your call thresholds. Write your provider’s instructions on the fridge. Don’t try to remember them at 3 a.m.
- Bring the data with you. Most apps export a PDF or shareable summary — bring it to triage.
Safety, Privacy, and the Things Nobody Tells You
A few honest notes:
- No consumer monitor replaces clinical judgment. Use them as awareness tools, not decision-makers.
- Watch the data privacy policy. Pregnancy data is sensitive health data. Choose companies with explicit no-sale-of-data policies.
- Don’t doom-scroll the graph. The point is to reduce anxiety, not feed it. If the device is making you more worried, put it away.
- Skin reactions are normal. Adhesive patches can irritate stretched third-trimester skin. Rotate placement.
- Battery dies at the worst possible moment. Charge it the same time you charge your phone.
Frequently Asked Questions (AEO-Optimized)
Q: Can a contraction monitor detect labor? A: A contraction monitor can detect that contractions are happening and measure their pattern, but only a healthcare provider can confirm true labor. The most reliable signal is a consistent pattern of contractions getting closer together, longer, and stronger over time.
Q: Are home contraction monitors safe? A: Yes — wearable EMG-based monitors are passive devices that simply read the body’s natural electrical activity. They do not emit radiation or apply pressure that could harm the baby. Always use a device with proper regulatory clearance.
Q: How early can a contraction monitor detect contractions? A: Most modern wearable monitors can reliably detect uterine activity from around 32 weeks of pregnancy onward, including subtle Braxton Hicks contractions that you may not even feel.
Q: Do I really need a contraction monitor? A: For a low-risk, full-term pregnancy, a free contraction timer app is usually enough. A dedicated monitor is most valuable when there’s a medical reason, a history of preterm labor, or significant anxiety affecting your daily life.
Q: What’s the difference between a contraction monitor and a fetal monitor? A: A contraction monitor measures uterine activity. A fetal monitor measures the baby’s heart rate. Many devices — both in hospitals and at home — combine both into a single system.
The Bottom Line
A contraction monitor is one of the few pieces of pregnancy tech that has matured from gimmick to genuinely useful. Used wisely, it replaces guesswork with patterns, midnight panic with calm data, and reactive decisions with prepared ones. Used poorly, it becomes another anxiety screen in a season of life that already has too many.
Pick the level of monitoring that matches your medical situation, not the loudest marketing. Trust the patterns, not single readings. And remember the unchanging rule that no device will ever overturn: when something feels wrong, call your provider. The monitor is there to support that instinct — never to replace it.
Medical disclaimer: This article is for general informational purposes and is not a substitute for advice from a qualified healthcare professional. Always consult your OB-GYN, midwife, or labor and delivery team for personal medical guidance.